Back Pain and Sciatica – Physical Therapy Treatments

This month I figured I’d post on a couple case studies related to back pain and sciatica, and how we evaluate and treat cases like this at Elite Physical Therapy. We’ve had a lot of great success with these folks so thought I’d share a couple examples.
Back pain, and associated leg pain, can be difficult to treat but we like a challenge! Playing detective can be fun if you know what to look for. Check out the pictures below that show the paths the spinal nerves take throughout the body. Leg pain (or what many people like to call ‘sciatica’) can follow a number of paths down the leg and sometimes that can be a dead give away to identify exactly where the pain is coming from.
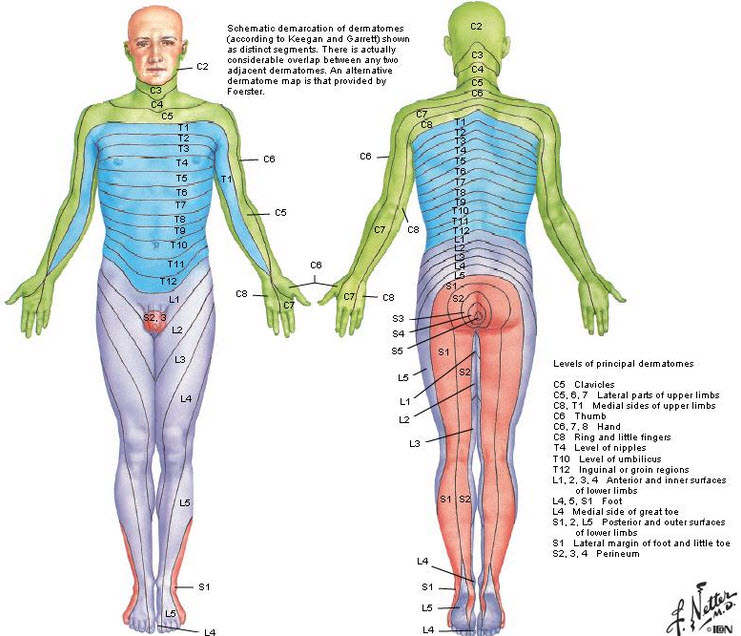
***The letter and numbers above correspond to a particular spinal nerve, i.e. L4 means lumbar spinal nerve #4 ***
There are other ways to narrow down the location of the problem as well:
- the muscles will be painful to palpation at a specific vertebral segment and may even refer pain down the leg when palpated with deeper pressure.
- reflexes may be diminished. A slow or non-existent patellar tendon reflex corresponds with lumbar spinal nerve #4.
- Muscles may test weaker on the affected side which may indicate an injury to a particular spinal level or nerve. An example of this would be weakness in the calf muscles (can’t lift up on to the toes) which are controlled by the first two sacral nerves (S1 and S2 on the chart).
So here’s a great example of a number of these factors all lining up and how quickly the pain and loss of function can be addressed.
Case Study #1
The patient in this case had left sided low back pain and pain running down through the back of her hip and leg to the mid-calf. She felt a ‘pop’ in her back and immediate leg pain as a result of pushing and twisting trying to put a heavy object in the back of her truck. She is an avid runner but even standing and walking significantly increase her pain after 10 minutes.
Exam
So here is what I found:
- Symptoms following the S1 and 2 dermatomes down the back of the left leg
- Increased muscle tone/spasm at the S1 and S2 levels of the spine, and these muscles are tender to palpation.
- ‘Springing’ or pushing down on the S1/S2 vertebrae reproduced the symptoms into the back of her hip/upper thigh.
- She could do only 12 calf raises on her left leg while doing 25 on the right side (this muscle corresponds with S1 and S2 nerves).
- Achilles reflexes normal (S1 reflex)
It’s nice when everything points back to a specific level or two like that. Doesn’t always work that way but when it does it makes me much more confident that we can knock this out quickly.
Treatment
In this case I chose to use dry needling to address the muscles at the S1 and S2 spinal levels on both sides of the spine. Once the needles were placed I attached an electrical stimulation unit and she just relaxed for 10 minutes. Dry needling in conjunction with e-stim are shown in the research to decrease tone within the muscles as well as alleviate pain through a number of local and global factors.
The patient was instructed in two exercises that had multiple purposes:
- decrease pain through relaxation of the over worked muscles of the back and anterior hip
- facilitate improved stability through the lumbar spine and pelvis
Pretty simple exercises that are beyond the scope of this article but lots of bang for your buck when they only take 5 minutes 2-3 x per day.
Results
The patient had near full resolution of symptoms for two days after the first session. Her exercises relieved her pain at home and she could walk as much as she wanted. She tried to run on the third day but was unable due to pain.
We repeated the same dry needling + e-stim treatment during the second visit and followed it up by progressing her exercise program.
The patient cancelled her appointment the next week as she reported being completely pain free and back to running.
Final Thoughts
Sometimes it just works that well but I certainly won’t make that guarantee in every case! Back pain and ‘sciatica’ cases can be quite complex but knowing how to put together all the puzzle pieces definitely helps.
That’s probably enough to wrap your head around for this time. Next month I’ll post another case study but with a different symptom presentation. In the meantime if you have any questions just shoot me an email: joe@elitepttc.com or call 231 421-5805.
